Why you Might Need a C-section if Your Baby is too big for Delivery
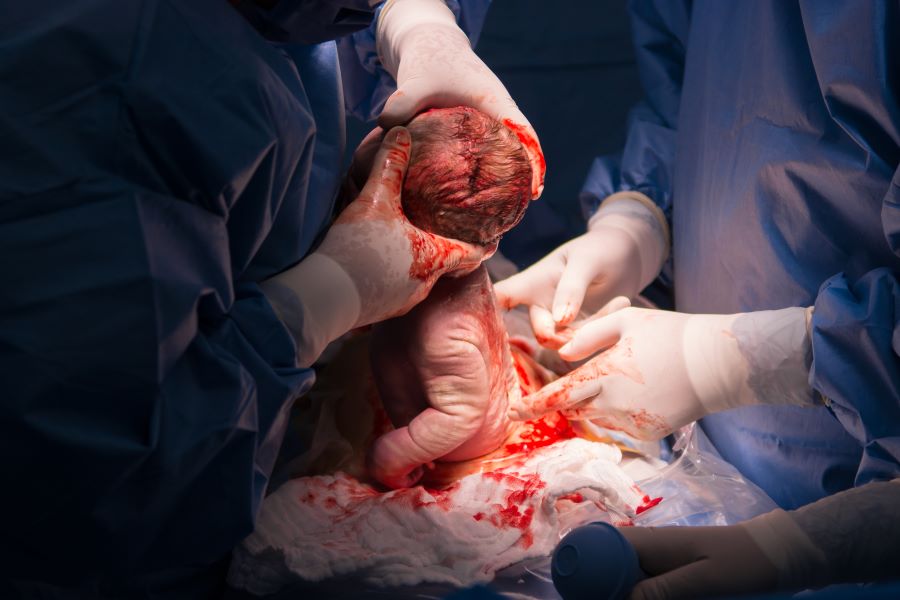

It is important to fully understand why a scheduled C-section is recommended as opposed to a trial of labor. While it is true that in some instances a C-section may be recommended, certain criteria should be used in making this decision to avoid unnecessary surgeries.
The term “macrosomia” refers to fetuses who are considered to weigh more than average. Most obstetric providers will use a cut-off of 4500 grams (or 9 pounds 15 ounces) to define fetuses as macrosomic. However, just because you are carrying a baby who is suspected to be macrosomic does not mean you should automatically sign up for a C-section.
In general, most obstetricians will recommend a scheduled C-section if your baby is estimated to weigh at least 5,000 grams (or 11 pounds) if you are not a diabetic. If you are a diabetic, that weight cut-off is decreased to 4,500 grams (or 9 pounds 15 ounces), and this is because babies born to diabetic mothers have increased fat and higher rates of shoulder dystocia at lower weights than compared to babies whose mothers are not diabetic.
This estimated fetal weight should be derived from a combination of physical exam and ultrasound measurements, so if your doctor is recommending a C-section solely based on how big your belly looks, you should ask about getting an ultrasound.
Keep in mind that if you are told you have a big baby but don’t meet the technical criteria where a C-section is recommended, attempting labor is the best way to find out if your baby will be able to deliver vaginally. If there are any concerns with how your labor is progressing, your doctor or midwife can then reassess if you do need a C-section, but many women have successfully delivered large babies vaginally with no issues—and have avoided unnecessary surgery (with the associated risks) in the meantime.
Powered by Bundoo®










































