My 15 Year old Hasn’t Started her Periods yet: Should I be Worried?
Dr. Kate Dudek • June 11, 2019 • 5 min read

- Around 2% of teenage girls do not start their periods before they are 15
- There are multiple reasons why a girl may start her periods later than others. Genetics, lifestyle and some medical conditions can contribute.
- Consider consulting a doctor for peace of mind if a teenage girl over the age of 15 shows no signs of puberty.
Most girls get their first period around the age of 12; this is usually about two years after the first signs of puberty. The medical name for starting your periods is menarche. Whilst 12 is the average, menarche can occur in girls as young as 8 years old. Furthermore, there is evidence that, particularly in some countries, the average age of puberty is falling.
Certainly, 200 years ago it was normal for a girl to start her periods between the ages of 15 and 17. However, nowadays that is the exception, rather than the norm; and up to 98% of girls will have started their periods before their fifteenth birthday.
So should you be worried if your daughter falls into the 2% of girls who have not yet started their periods?
The answer is, probably not. Some teenagers are just ‘late bloomers’ and, as the age of puberty tends to have a familial component, if you started your periods later than many of your friends, it is likely that your daughter will experience a similar thing.
Lifestyle factors affect when periods start
Lifestyle factors can also play a role. Being overweight or underweight can delay the start of puberty, as can excessive exercise. This is why ballerinas and gymnasts very often start their periods later than their counterparts. Having an eating disorder or suffering from intense stress can also delay menstruation. For any of these factors, resolving the underlying issue should rectify the issue; for example:
- Finding a healthy way to lose or gain weight.
- Reducing the intensity of an existing exercise schedule.
- Identifying and acting to resolve the things that are causing stress.
Medical issues can contribute to delayed puberty
In some cases there will be an underlying medical issue. Some cancer treatment might delay or prevent puberty from occurring. There may be a structural problem whereby part of the reproductive system is missing or blocked; endometriosis, characterised by the build up of endometrial deposits outside of the uterus, is probably the most well known structural impediment to normal reproductive function. A congenital condition called Müllerian agenesis results in complete or partial absence of parts of the uterus and vagina.
Other genetic disorders, including Turner syndrome can delay puberty, as can problems with the hypothalamus or pituitary gland. Hypothalamic dysfunction that occurs before puberty often resolves itself over time. Another medical complication that can cause girls to fail to have regular menstrual cycles is polycystic ovary syndrome (PCOS). Research has shown that girls with clinically-diagnosed PCOS often start their periods earlier or later than average. Furthermore, PCOS regularly causes menstruation disturbances, such as irregular periods, which can be exacerbated in those who have only just been through puberty.
Any of these medical conditions will need to be diagnosed by a doctor, who will then be able to offer advice on the best way of managing the symptoms.
What to do if a 15 year old has not started her periods
The age at which a girl starts her periods is influenced by a combination of genetic markers (predispositions) and environmental factors such as diet and exercise. To date, the research and clinical community has limited data on which specific genes are involved; however, with the advent of genome-wide association studies (GWAS), potential genetic targets can be identified and explored further.
More research is needed to understand the factors contributing to the timing of menstruation.
If your daughter has not had her first period by the age of 15 you may wish to consult a doctor for peace of mind, particularly if she has none of the typical signs of puberty. If, however, her breasts have started to form and she is developing pubic hair, it is very likely that her periods will start in the near future.
Nabta is reshaping women’s healthcare. We support women with their personal health journeys, from everyday wellbeing to the uniquely female experiences of fertility, pregnancy, and menopause.
Get in touch if you have any questions about this article or any aspect of women’s health. We’re here for you.
Sources:
- Carroll, Jessica, et al. “Environmental and Genetic Factors Influence Age at Menarche in Women with Polycystic Ovary Syndrome.” Journal of Pediatric Endocrinology and Metabolism, vol. 25, no. 5-6, 19 Apr. 2012, pp. 459–466., doi:10.1515/jpem-2012-0047.
- Karapanou, Olga, and Anastasios Papadimitriou. “Determinants of Menarche.” Reproductive Biology and Endocrinology, vol. 8, no. 1, 30 Sept. 2010, p. 115., doi:10.1186/1477-7827-8-115.
- Müller, Jørn. “Disturbance of Pubertal Development after Cancer Treatment.” Best Practice & Research Clinical Endocrinology & Metabolism, vol. 16, no. 1, Mar. 2002, pp. 91–103., doi:10.1053/beem.2002.0183.
- Practice Committee of American Society for Reproductive Medicine. “Current Evaluation of Amenorrhea.” Fertility and Sterility, vol. 90, no. 5 (suppl.), Nov. 2008, pp. S219–S225., doi:10.1016/j.fertnstert.2008.08.038.
- “Delayed Periods.” NHS, www.nhs.uk/conditions/periods/delayed-periods/.
Download the Nabta App
Related Articles

Why Does my Toddler Want to be Naked? (2024)
Find out why toddler want to be naked and get simple tips to manage it calmly, including sensory needs, new skills, and setting routines, The toddler years are marked by a variety of developmental milestones, one of which is the ability to dress and undress independently. While this new skill can be exciting for children, it can often [lead](https://nabtahealth.com/glossary/lead/) to inconvenient or embarrassing situations for parents, such as toddlers wanting to be naked all the time. However, this behavior is quite common and typically not a cause for concern. Why Toddlers Want to Be Naked ----------------------------- * **Sensory Input:** The main possible reasons toddlers like to keep naked include sensory input. Clothing such as seams within socks or shirt tags may be uncomfortable for a child, and this sensation of discomfort may make them remove their clothes frequently. If you suspect the child is extremely sensitive to a trivial input, it may indicate a problem like sensory processing disorder, for which the pediatrician can be consulted. * **Undressing as an Achievable Developmental Milestone**: One needs to consider that this might be one of the primary ways a toddler achieves a milestone in their development. They may feel proud of their new skill and want to share it with others, no matter how frustrating this may be for the parent. * **Attention Seeking**: The toddler may sometimes undress for attention; this is particularly true if the parent responds strongly to the behavior. The reaction from a frustrated or embarrassed parent may elicit persistence in undressing with the child to get some form of response. This, therefore, means that how parents react significantly influences behavior. How to Handle Your Toddler’s Nakedness -------------------------------------- * **Stay calm**: Parents should not react humiliatingly to the child instead of getting angry but may respond calmly with no humiliating remarks. The parents may tell their children how good they are at undressing and ask them to wear their clothes. This should be responding neutrally to avoid further exaggeration of the behavior. You might try dialogue like, “Wow! Terrific. I can see you undress yourself like a big kid. Can you get dressed now and show me how you do that?” By acting like the undressing is no more of a big deal than dressing, this may stop the problem in its tracks. * **Allocate Times to be Undressed**: At times, parents will find it beneficial to establish times when the toddler can be undressed, such as in preparation for bath time or within the confines of the home. More often than not, these organized opportunities will enable toddlers to feel less anxious and content with the parameters that have been established. * **Remember, It’s Just a Phase**: Like most [phases of development](https://nabtahealth.com/article/qa-with-raquel-anderson-brain-development-in-a-12-month-old/), the compulsion to be naked shall pass. Children do appear to grow out of it eventually, and parents need a little patience and understanding. **References:** 1.A. R. Turner, P. S. Thompson, “Sensory Processing and the Toddler Years: A Study of Early Childhood Sensory Experiences,” Journal of Developmental Psychology, 2023. 2.M. E. Calloway, J. L. Roberts, “Undressing as a Developmental Milestone in Early Childhood,” Infant and Toddler Development Journal, 2024. 3.S. D. Harris, “Understanding Toddler Behavior: Reactions to Nakedness and Sensory Sensitivity,” Parenting Psychology Quarterly, 2024. 4.L. B. Wilkins, “How to Respond to Common Toddler Behaviors: Positive Guidance Techniques,” Journal of Child Development and Parenting, 2023. **Sources:** * What To Expect * Undressing (preferring to be naked). [American Academy of Pediatrics](https://www.aap.org/) * Emotional Development in Preschoolers. Powered by Bundoo®

Fact or Fiction: Garlic Oil Helps Cure Ear Infections 2024
Garlic oil helps cure ear infections, natural [treatments](https://nabtahealth.com/) such as garlic oil are highly recommended as possessing antibacterial and antiviral properties. But does garlic oil live up to its reputation? The Science Behind Garlic and Ear Infections -------------------------------------------- Garlic has been used as a natural remedy for several centuries to cure various infections, among other ailments. The active ingredient, allicin, has been shown to exhibit antibacterial and antiviral properties that can help with the symptoms of an ear infection. A few studies confirm that allicin decreases the presence of certain bacteria and viruses, thus assisting in resolving the ear infection sooner. Yet anatomically, the ear makes this problematic as the tympanic membrane, or eardrum, acts to prevent direct delivery of oil or drops to the area of the middle ear where infections occur. 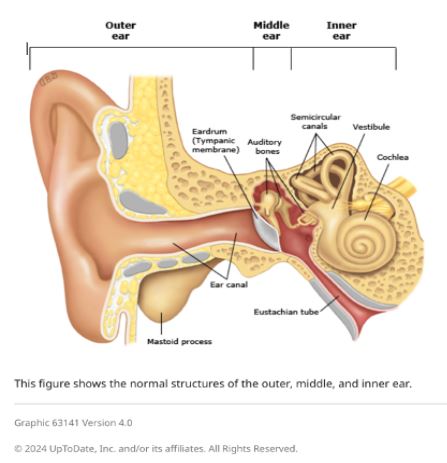 Evidence of Garlic Oil and Herbal Remedies ------------------------------------------ Studies on garlic oil, often combined with other herbs such as mullein, demonstrate it can decrease ear pain. A review published in 2023 reported that herbal ear drops, including those containing garlic, relieved pain in subjects with acute otitis media. However, researchers pointed out that while garlic oil may grant some advantages in the feeling of discomfort, its effect on the infection is limited by the eardrum barrier. Most infections will still self-resolve, but garlic oil can offer a natural alternative for pain management. Some studies in 2023 and 2024 also report that herbal extracts, including garlic, reduce dependence on heavy pain medications. Garlic is relatively cheaper and easier to access in herbal drops, particularly in many settings where prescription ear drops are not available. Safety and Proper Application of Garlic Oil ------------------------------------------- Being a potentially palliative resource, garlic needs to be used in the right manner. Experts advise against putting pure or undiluted garlic oil into the ear, as this can be too harsh and thus irritate or even injure sensitive ear tissue. Garlic extracts in commercially prepared herbal ear drops are recommended for use in the ear. In these products, garlic would have been diluted to safe levels while still being beneficial. Seeing a Health Professional ---------------------------- Consulting a health professional beforehand is very important when using garlic oil or any other herbal remedy against ear infections. Sometimes, ear infections result in complications, especially when not treated properly, and might cause recurrence. A healthcare provider will best help assess whether garlic oil or any other remedy may be indicated for each case and may recommend the safest treatment. Possible Benefits of Garlic Oil for Ear Health ---------------------------------------------- * Natural Pain Relief: Garlic oil’s antimicrobial and anti-inflammatory action soothes ear pain. * Cost-Effective: Garlic-based herbal remedies are generally cheaper than several prescription-based ear drops. * Readily Available Option: Garlic oil is readily available at health stores and can be ordered online. Current Research and Future Directions -------------------------------------- Herbal remedies, such as garlic oil, are still under research, especially for their role in pain relief and supporting natural recovery in light ear infections. Other studies investigate more advanced formulations that could let active compounds bypass the eardrum more effectively, thus giving a chance for enhanced effectiveness against middle-ear infections without the use of antibiotics. Key Takeaways ------------- * In effect, it has a minimal impact on the infection. It does not cure the disease but helps with earache because the membrane prevents the oil from reaching the middle ear. * Only use mild formulations. Commercially prepared herbal ear drops are very good compared to undiluted garlic oil. This is done to prevent irritation. * Consult a professional. Consult your health provider before this natural remedy, especially if you have recurring symptoms. References 1.Johnson, L., & Patel, R. (2023). [The Role of Herbal Remedies in Treating Ear Pain](https://pubmed.ncbi.nlm.nih.gov/): A Focus on Garlic Oil. Journal of Complementary Medicine, 61(2), 102-115. 2.Sharma, D., & Lee, H. (2024). Evaluating Garlic Extract for Natural Pain Relief in Ear Infections. Advances in Integrative Health, 42(1), 89-99. 3.Verhoeven, E., & Kim, S. (2023). Garlic and Herbal Extracts in Ear Infection Management. Health and Wellness Journal, 23(4), 167-178.

7 Healthy Eating Tips for Postpartum Weight Loss In 2024
Your new baby has arrived, and you are eager to get back into shape. However, [losing weight after pregnancy](https://nabtahealth.com/articles/7-healthy-eating-tips-for-postpartum-weight-loss/) takes time and patience, especially because your body is still undergoing many hormonal and metabolic changes. Most women will lose half their baby weight by 6-weeks postpartum and return to their pre-pregnancy weight by 6 months after delivery. For long-term results, keep the following tips in mind. Prior to beginning any diet or exercise, [please consult with your physician](https://nabtahealth.okadoc.com/). 1\. **Dieting too soon is unhealthy.** Dieting too soon can delay your recovery time and make you more tired. Your body needs time to heal from labor and delivery. Try not to be so hard on yourself during the first 6 weeks postpartum. 2\. **Be realistic**. Set realistic and attainable goals. It is healthy to lose 1-2 pounds per week. Don’t go on a strict, restrictive diet. Women need a minimum of 1,200 calories a day to remain healthy, and most women need more than that — between 1,500 and 2,200 calories a day — to keep up their energy and prevent mood swings. And if you’re nursing, you need a bare minimum of 1,800 calories a day to nourish both yourself and your baby. 3\. **Move it**. There are many benefits to exercise. Exercise can promote weight loss when combined with a reduced calorie diet. Physical activity can also restore your muscle strength and tone. Exercise can condition your abdominal muscles, improve your mood, and help prevent and promote recovery from postpartum depression. 4\. **Breastfeed**. In addition to the many benefits of breastfeeding for your baby, it will also help you lose weight faster. Women who gain a reasonable amount of weight and breastfeed exclusively are more likely to lose all weight six months after giving birth. Experts also estimate that women who breastfeed retain 2 kilograms (4.4 pounds) less than women who don’t breastfeed at six months after giving birth. 5\. **Hydrate**. Drink 8 or 9 cups of liquids a day. Drinking water helps your body flush out toxins as you are losing weight. Limit drinks like sodas, juices, and other fluids with sugar and calories. They can add up and keep you from losing weight. 6. **Don’t skip meals**. Don’t skip meals in an attempt to lose weight. It won’t help, because you’ll be more likely to binge at other meals. Skipping meals will also make you feel tired and grouchy. With a new baby, it can be difficult to find time to eat. Rather than fitting in three big meals, focus on eating five to six small meals a day with healthy snacks in between. 7\. **Eat the rainbow.** Stock up on your whole grains, fruits, and vegetables. Consuming more fruits and vegetables along with whole grains and lean meats, nuts, and beans is a safe and healthy diet. ose weight after postpartum Is one of the biggest challenge women face worldwidely. Different Expertise and studies indicated that female might lose approximately 13 pounds’ weight which is around 6 KG in the first week after giving birth. The essential point here is that dieting not required for losing the weight, diet often reduce the amount of some important vitamins, minerals and nutrients. **Here are seven tips from the professional nutritionist perspective that can be considered for losing weight after postpartum these are;** 2\. Considered food like fish, chicken, nuts, and beans are excellent sources of protein and nutrients. 3\. A healthy serving of fat, such as avocado, chia seeds or olive oil 4\. With the balance diet please consider to drink plenty of water to stay hydrated. 5\. Regular exercise helps to shed extra pounds and improve overall health. 6\. Fiber-rich foods should be included to promote digestive health and support weight loss efforts. 7\. Don’t forget about self-care. By making these dietary changes and incorporating physical activity, you can achieve postpartum weight loss sustainably and healthily. **Sources:** * Center for Disease and Control and Prevention * Healthy Weight: it’s not dieting, it’s a lifestyle. Obstetrics and Gynecology * The risks of not breastfeeding for mothers and infants. The American College of Obstetrics and Gynecologists * Guidelines of the American College of Obstetricians and Gynecologists for exercise during pregnancy and the postpartum period. Powered by Bundoo®

