كيف تُؤثّر الجذور الحرة على الجلد ؟
Free radicals are produced by the body and are found pretty much everywhere. Like many things in life they are fine in moderation. In fact, they can play a protective role, helping the body to respond to stress and protecting against harmful microbes. They also play a role in the breakdown of polyunsaturated fatty acids.
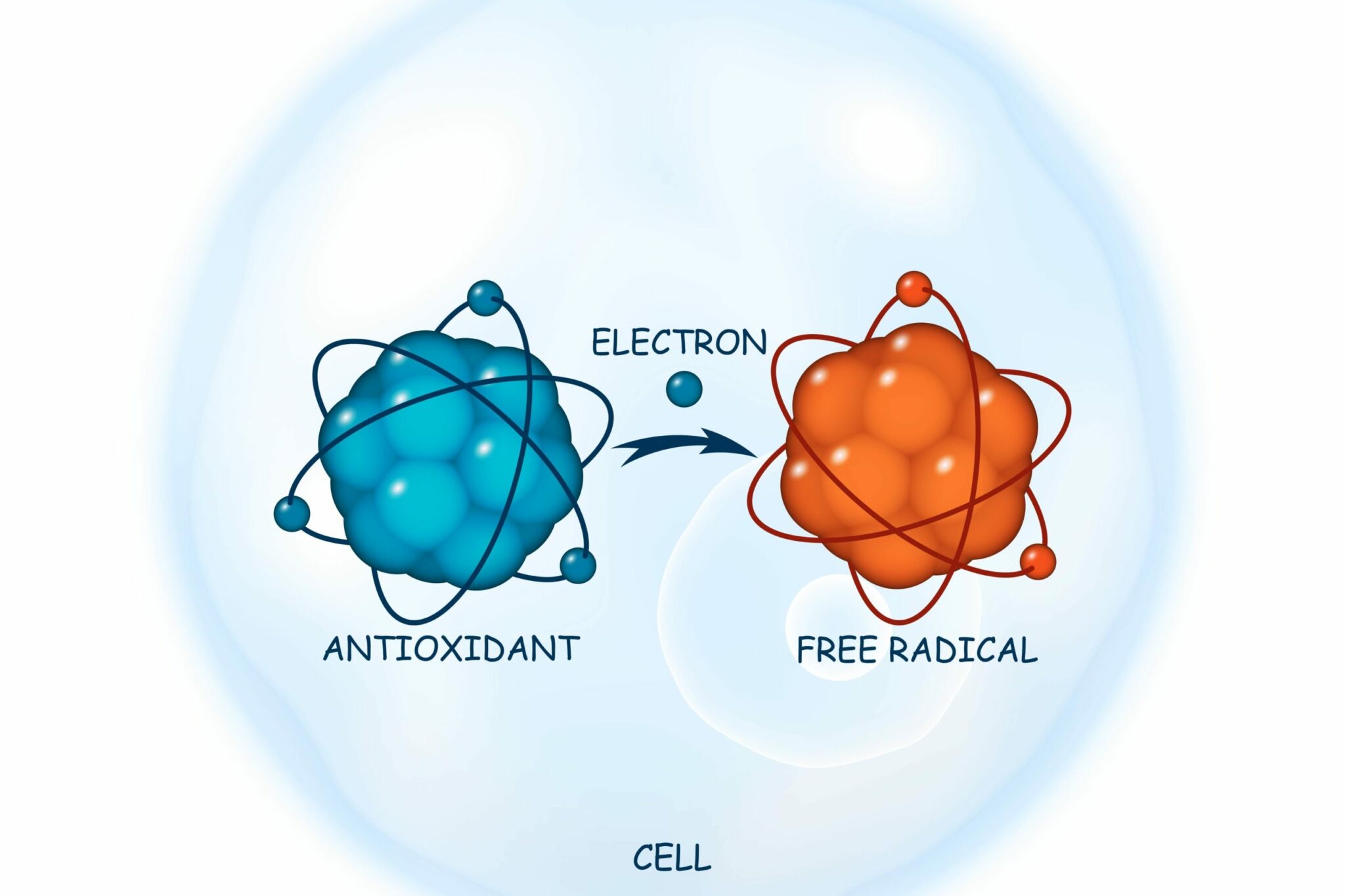
However, too many of them can rapidly have a detrimental effect, triggering oxidative stress and rendering the body unable to counteract the harmful effects caused by their presence. This is because they are unstable molecules which lack an electrode and, thus, they exist in a perpetual state of attempting to ‘fill the gap’.
How does the body counteract the potentially damaging effects of free radicals?
During normal cellular metabolism, in addition to this, the cells of the body produce antioxidants. These are also present in the foods we eat and, often, in the products we apply as part of our daily skincare routine. The great thing about antioxidants is that they are stable and can donate electrons. This neutralises the circulating free radicals, reducing their capacity to cause damage.
What happens if the balance between free radicals and antioxidants is disrupted?
Most free radical-induced damage occurs when the balance between their production and the availability of antioxidants is disrupted. If there is an excess of unstable it that cannot be neutralised, they will end up oxidising the DNA and proteins of otherwise healthy cells, causing oxidative stress and predisposing the cells to further damage. The imbalance between free radicals and antioxidants puts the body into a stressed state and, as a result, more free radicals are produced. This renders more cells vulnerable to oxidative stress and can ultimately compromise normal cellular activity.
Where do free radicals come from?
Free radicals are endogenously produced by the body, but they are also induced by pollution, sunlight and smoking. Other triggers include ionising radiation and toxic chemicals (including chemotherapeutic agents).
Unfortunately, cancer cells also produce high numbers of free radicals. This puts cancer patients at particular risk of suffering from the detrimental effects of excess free radicals, as not only are their bodies producing more, but their treatment is likely to be exacerbating this effect. There is no direct evidence that antioxidants are anti-carcinogenic; however, they do seem to alleviate some of the symptoms of excess free radical accumulation.
Free radicals and the skin
One of the most visible signs of free radical-induced damage is premature aging of the skin, as well as inflammation and irritation. Dry, painful skin is very frequently observed as a side-effect of cancer treatment. The antioxidants produced naturally by the body do help to combat these effects, however levels decline with age, leaving the body’s cells and DNA vulnerable to damage.
Many of the skincare products in use today contain antioxidants to supplement the body’s natural supplies. In fact, ‘antioxidant’ has become something of a buzz word within the beauty industry, with many companies now choosing to include antioxidants not only in their formulations, but also in their marketing campaigns.
An ideal antioxidant supplement will not only restore health and combat the aging effects of too many free radicals, but will also indirectly retain skin moisture and elasticity by reducing collagen degradation caused by free-radicals in the tissues.
Some of the most frequently used antioxidants in beauty products are vitamin C, retinol (vitamin A), vitamin E, resveratrol, coenzymeQ10 and glutathione. Vitamin E is found in abundance in natural plant-based oils.
Try using the treat pack and the clean on-the-go pack, incase of dry skin.
Sources:
- Dröge, W. “Free Radicals in the Physiological Control of Cell Function.” Physiological Reviews, vol. 82, no. 1, Jan. 2002, pp. 47–95., doi:10.1152/physrev.00018.2001.
- Petersen, R C, et al. “Advancements in Free-Radical Pathologies and an Important Treatment Solution with a Free-Radical Inhibitor.” SF Journal of Biotechnology and Biomedical Engineering, vol. 1, no. 1, 2018, pp. 1003.
- Tafani, M, et al. “The Interplay of Reactive Oxygen Species, Hypoxia, Inflammation, and Sirtuins in Cancer Initiation and Progression.” Oxidative Medicine and Cellular Longevity, 2016, doi:10.1155/2016/3907147.










